


Theme
Simulation and Simulated Patients
Category
Simulation
INSTITUTION
Cardiff University and Aneurin Bevan Health Board

-
Non-technical skills (NTS) are essential for patient safety1 and their integration into the medical curriculum has been recommended.
-
NTS teaching is currently limited in the undergraduate curriculum.
-
NTS were first defined in the 1970’s when investigations into air crashes deduced that the disasters occurred not due poor technical skills, but due to poor teamwork, communication and other skills1.
-
NTS were transferred to healthcare through the development of an anaesthetists’ rating system in the early 2000’s and have since been highlighted for surgeons, intensivists, scrub practitioners and acute medical teams.
Aims
-
To identify NTS required by medical students.
-
To develop a simulation-based teaching programme to train medical students in NTS.
Method
- Previous taxonomies (anaesthetists NTS (ANTS)2 and NTS for surgeons (NOTSS)3) were reviewed along with articles from a literature search containing the keywords “non-technical skills”.
-
A 9-week participant-observation was then done - observing junior doctors, anaesthetists and NTS teaching, and identifying commonly-used NTS.
-
A medical students’ taxonomy (MS-NTS) was then created, and a simulation-based teaching programme developed for medical students in years 2–5.
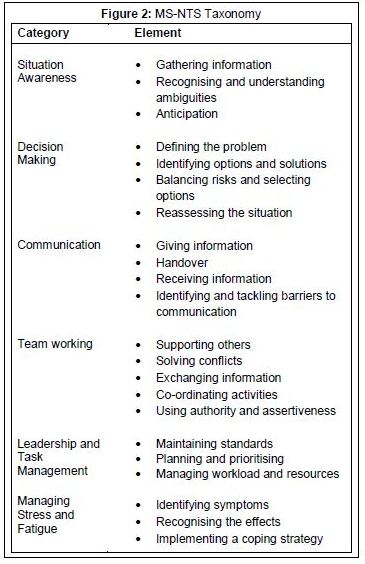
- Most NTS were observed during the participant-observation placement, reinforcing the necessity for NTS training. The final MS-NTS taxonomy created as a result of participant-observation is shown in figure 2.
- Simulation is most effective for NTS training as students value the safe learning experience and respond positively. NTS understanding and development is maximised by effective feedback. Three stages are recommended in NTS training: (1) awareness, (2) practice and feedback and (3) reinforcement. This strategy was incorporated into a simulation-based teaching programme, designed to cover the basic training objectives outlined in figure 3.
- Eight students at a time will attend a two-hour NTS teaching session. Students are made aware of NTS by an introduction by the tutor, where students are also encouraged to share their experiences and observations of NTS seen on clinical placements.The practice and feedback stage involves 4 scenarios based on critical or acute medical scenarios, run on a full-size simulator, each ten minutes long and managed by two students using the NTS principles. The students ‘hand the patient over’ to the tutor at the end of the scenario and undertake a ten-minute feedback session. Reinforcement is provided by yearly sessions, starting in year 2. Students will be given a student handbook and a student logbook in which to reflect upon the NTS sessions and NTS observed on clinical placements.
- The students will also be assessed using a 6-point NTS rating system.
-
There are limitations to the teaching programme:
- Simulators are expensive and must be contained in custom-built or modified facilities.
- Time is required to run the programme.
- Tutors and simulator operators will require training.
- It has been suggested that NTS teaching is incorporated into the undergraduate medical curriculum.
- Following incorporation, further research will be needed to evaluate its effectiveness and whether it can be integrated into clinical placements.
- Incorporation of NTS teaching into the medical curriculum is highly recommended.
- Simulation is an effective method of teaching NTS.
Many thanks to Dr R Rouse, Consultant Anaesthetist, Nevill Hall Hospital, Abergavenny and to all the other anaesthetists at Nevill Hall who assisted in this project.
- Engel N, Patey E R, Ross S, Wisely L. Non-technical skills. sBMJ. 2008; 16: 454-455.
- Fletcher G, Flin R, McGeorge P, Galvin R, Maran N, Patey R. Rating non-technical skills: developing a behavioural marker system for use in anaesthesia. Cogn Tech Work. 2004;6:165-171
- Yule S, Flin R, Paterson-Brown S, Maran N, Rowley D. Development of a rating system for surgeons’ non-technical skills. Medical Education. 2006;40:1098-1104.
- Reader T, Flin R, Lauche K, Cuthbertson B H. Non-technical skills in the intensive care unit. Br J Anaesth. 2006; 96 (5): 551-559.
.JPG)
 Send Email
Send Email