


Theme
Simulators and Simulation
Category
Simulation
INSTITUTION
Royal Preston Hospital, Lancashire Teaching Hospitals Trust

Simulation training provides a platform for trainees to hone skills that may be called into use infrequently; major burns are an ideal topic because of their rarity, significant morbidity and mortality, and the requirement for A&E, anaesthetics and plastic surgery trainees to be proficient in the stabilisation and initial resuscitation of these patients.
Further work is already being done to incorporate a multidisciplinary team element. Currently scenarios have been developed to include Emergency Department (ED), Anaesthetics, and Plastic Surgery and Burns trainees as well as nursing staff.
An assessment tool has been proposed and is in the initial stages of development. This is an important aspect of any educational tool given the modern pressures on training and revalidation.
Training in emergency burn management is commonly delivered in a moulage format largely thanks to the success of the Emergency Management of Severe Burns (EMSB) course; this course has become the standard for training within the UK.
Simulation training has seen huge advances in the last few years. Not least because of the ever increasing pressures on trainee time as well as an increasing focus on learning new and potentially life saving skills away from the bedside.
Burns care is ideal for simulation based training as a result of its acute nature, fairly predictable initial pathophysiology and its relative infrequency; the National Burns Care Review 2001 estimated that 1,000 patients are admitted to UK hospitals with severe burns per annum1.
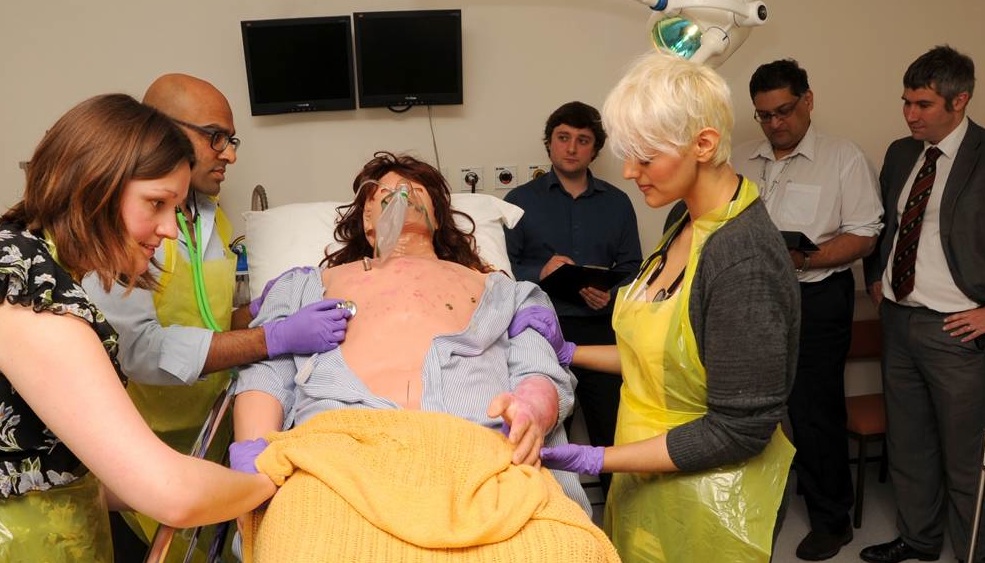
Fig 1. Trainees assessing a manikin mocked up with burn make-up in the simulation suite with three assessors in the background.
An educational programme for plastic surgery and burns trainees was devised and delivered using a state of the art high-fidelity simulation training facility at the Lancashire Simulation Centre.
The aim of the project was to incorporate the application of clinical knowledge and technical skill but also the human factors elements, or non-technical skill that can impact upon clinical effectiveness.
Several scenarios were devised with the key skills identified including, decision-making, teamwork, communication, clinical leadership, and ultimately the application of clinical skills. An initial pilot session was delivered in November 2011 and a subsequent session in May 2012 for several “early trainees” and “registrars” in the plastic surgery department.
Two consultant plastic surgeons assessed trainees in real time within the facility. Each scenario was followed by a trainee lead video de-brief focusing on human factors elements and clinical acumen.
Participant feedback on the session was given anonymously at the end of each session and the data collated.
Severe burns education is ideally suited to Human Patient Simulator training.
The scope of the project has been extended by involving the wider multi-disciplinary team and by creating an assessment tool.
High-fidelity simulation may hold the key to standardising burns care and education.
Special thanks to Mark Pimblett and Lorna Lees at Lancashire Simulation Centre as well Mrs Jackie Hanson and all the participants who have thus far contributed to our work.
Trainees found simulation training to be an excellent adjunct to current methods of learning in burns and human factors. Collated participant feedback revealed that 100% of trainees felt that they would recommend the course to others and that they would like more simulation training incorporated into their own education.
Feedback Summary:
|
|
Participant response
(n=11) |
|
|
Simulation themed feedback |
Yes |
No |
|
1. Is this your first experience of human patient simulation? |
86% |
14% |
|
2. The use of human patient simulation enhanced my learning experience:
|
100% |
- |
|
Educational themed feedback |
Yes |
No |
|
3. Was the content suited to your educational requirements? |
100% |
- |
|
4. This session has enhanced my ability to manage acute severe burns: |
100% |
- |
|
Course themed feedback |
Yes |
No |
|
5. Would you recommend this course to others? |
100% |
- |
|
6. Should simulation training be incorporated into plastics and burns curriculum and formal training? |
100% |
- |
Fig 3. Tabulated results of participant feedback following simulation training
1. National Burn Care Review Committee. Standards and strategy for burn care. ; 2001j
2. The Australian and New Zealand Burn Association. Emergency Managament of Severe Burns Course Manual. 2006
3. Stone CA, Pape SA. Evolution of the emergency management of severe burns (EMSB) course in the UK. Burns 1999, May;25(3):262-4
4. Black SA, Nestel DF, Kneebone RL, Wolfe JHN. Assessment of surgical competence at carotid endarterectomy under local anaesthesia in a simulated operating theatre. The British Journal of Surgery 2010, Apr;97(4):511-6
5. HOSLER RM. Six years' experience with the cleveland cardiac resuscitation course. AMA Arch Surg 1956, Nov;73(5):813-9
6. Donoghue AJ, Durbin DR, Nadel FM, Stryjewski GR, Kost SI, Nadkarni VM. Effect of high-fidelity simulation on pediatric advanced life support training in pediatric house staff: A randomized trial. Pediatr Emerg Care 2009, Mar;25(3):139-44
7. Brydges R, Carnahan H, Rose D, Rose L, Dubrowski A. Coordinating progressive levels of simulation fidelity to maximize educational benefit. Academic Medicine : Journal of the Association of American Medical Colleges 2010, May;85(5):806-12
8. Abrahamson S, Denson JS, Wolf RM. Effectiveness of a simulator in training anesthesiology residents. Academic Medicine 1969;44(6):515
9. Donoghue A, Nishisaki A, Sutton R, Hales R, Boulet J. Reliability and validity of a scoring instrument for clinical performance during pediatric advanced life support simulation scenarios. Resuscitation 2010, Mar;81(3):331-6
10. Donoghue A, Ventre K, Boulet J, Brett-Fleegler M, Nishisaki A, Overly F, et al. Design, implementation, and psychometric analysis of a scoring instrument for simulated pediatric resuscitation: A report from the EXPRESS pediatric investigators. Simul Healthc 2011, Apr;6(2):71-7
11. Savoldelli GL, Naik VN, Hamstra SJ, Morgan PJ. Barriers to use of simulation-based education. Can J Anaesth 2005, Nov;52(9):944-50
12. Reznick RK, MacRae H. Teaching surgical skills--changes in the wind. The New England Journal of Medicine 2006, Dec;355(25):2664-9
13. Kalson NS, Jenks T, Woodford M, Lecky FE, Dunn KW. Burns represent a significant proportion of the total serious trauma workload in england and wales. Burns 2012;38(3):330 – 339
14. Bond WF, Lammers RL, Spillane LL, Smith-Coggins R, Fernandez R, Reznek MA, et al. The use of simulation in emergency medicine: A research agenda. Acad Emerg Med 2007, Apr;14(4):353-63.
15. Rudolph JW, Simon R, Raemer DB, Eppich WJ. Debriefing as formative assessment: Closing performance gaps in medical education. Acad Emerg Med 2008, Nov;15(11):1010-6.
16. Issenberg SB, McGaghie WC, Petrusa ER, Lee Gordon D, Scalese RJ. Features and uses of high- fidelity medical simulations that lead to effective learning: A BEME systematic review. Med Teach 2005, Jan;27(1):10-28.
 Send Email
Send Email