


Theme
Simulation
INSTITUTION
Clinical Skills Center, Medical University of Graz

Basic and advanced life support (ALS) are extensively taught during the clinical period of medical study. Yet, the practical ALS competence of graduating students is still insufficient (Weller et al. 2004; Jensen et al. 2008). A possible solution may be to implement advanced emergency skills training in the pre-clinical period of study.
A two-hour course teaching cardiopulmonary resuscitation, airway management procedures (e.g. oropharyngeal suctioning, use of supraglottic airway devices) and structured emergency assessment was implemented.
Central components are:
- thorough theoretical pre-course preparation
- student peer-teaching
- small teaching groups
- a hands-on concept.
Simulation technology is used throughout the entire course:
- part-task trainers and static manikins for procedural training
- a simulation software for the practice of patient assessment
- high-fidelity patient simulators for emergency simulations.
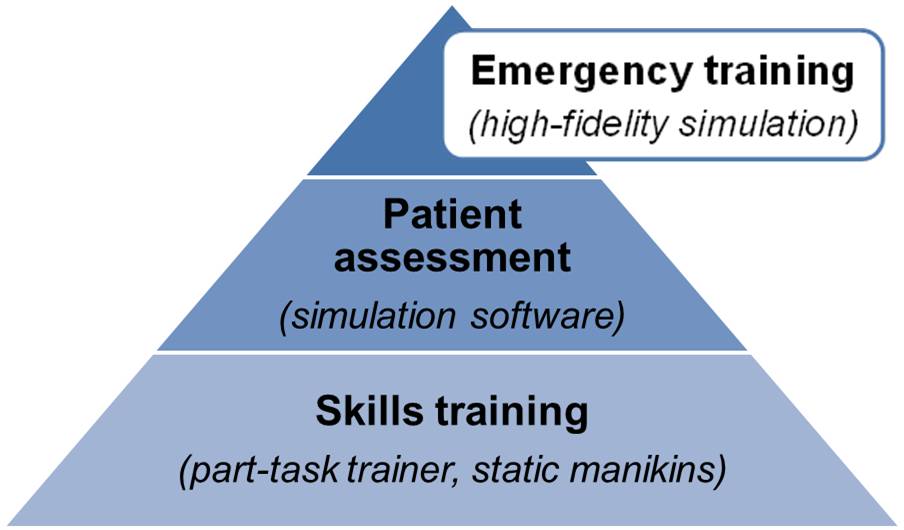
Figure 1: Course structure
Between November 2011 and February 2013, 398 students have successfully completed the course. Initial student satisfaction is very high: 51 students have participated in a voluntary online-evaluation, with 45 students (88.2%) strongly agreeing/agreeing that they were satisfied with the course (mean grade of 1.4±1.0 on a six-point Likert scale).
.jpg)
Figure 2: Student satisfaction
By using an innovative simulation-based course design, advanced practical aspects of emergency medicine can be implemented successfully in pre-clinical student education. However, despite high student satisfaction (Kirkpatrick hierarchy level I), students’ post-course skills competence (Kirkpatrick hierarchy level II) and the long-term impact of this single training have to be further investigated (Kirkpatrick & Kirkpatrick 2006; ten Cate et al. 2010).
1) Pre-clinical students are highly satisfied with advanced emergency skills training.
2) Manifold simulation-based approaches are valuable in teaching first-year students emergency skills.
 Send Email
Send Email