


Theme
Postgraduate Education
INSTITUTION
London Specialty School of Obstetrics and Gynaecology
Professional Support Unit, Shared Services, Health Education London

Burnout is a psychological term for the negative response to chronic, job-related emotional stress.
It is a three-dimensional syndrome of: Emotional Exhaustion (EE), Depersonalisation (DP) and a Lack of Personal Accomplishment (PA).
Traditionally, it is thought to occur more in people working in human service professions. For example: teachers, police officers, social workers, nurses and doctors.
Studies have demonstrated that doctors who suffer from Burnout are more likely to experience depression, drink alcohol to harmful levels, take prolonged sick leave and plan retirement early (1). It is well known that medical trainees suffering from Burnout consider changing specialty or leaving medicine entirely (2). Whilst it is obvious that Burnout is detrimental to the well-being of doctors, these issues inevitably impact on patient care and safety. Research demonstrating an increase in medical prescribing errors, decreased medical knowledge and learning, communication skills, professionalism and commitment to the job is well-documented across all specialties, all grades and all healthcare systems in different parts of the world (3).
Results 1. MBI Scores in GP, Paediatric and O&G doctors-in-training
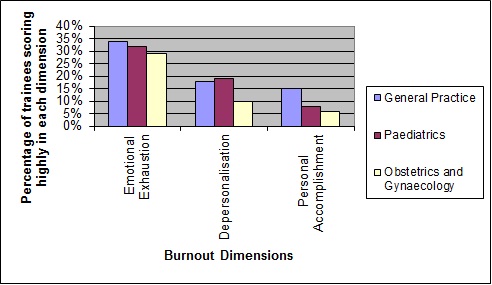
Graph showing percentage of trainees in each run-through training specialty experiencing high levels of EE, DP, PA
Results 2. Personality factors and MBI dimensions in run-through trainees
1. Scoring highly on neuroticism was significantly associated with elevated emotional exhaustion and depersonalisation scores.
2. Scoring highly on agreeableness and conscientiousness were significantly associated with lower emotional exhaustion and depersonalisation scores
3. Suffering with a lack of personal accomplishment was significantly associated with high scores of neuroticism and low scores of agreeableness and conscientiousness.
Aims:
1. To examine whether first year trainees from 3 run-through specialties (obstetrics and Gyanecology (O&G), General Practice (GP) and Paediatrics) suffer from Burnout.
2. To examine the association between Burnout and specific personality and work related factors.
Method:
An online web-based survey was emailed to 604 London regional trainees in their first year of O&G, GP and Paediatric training. The demographic data was reported anonymously. A 5 factor personality measure was used detailing agreeableness, conscientiousness, extraversion, neuroticism and openness. The 3 dimensions of Burnout were measured using the Maslach Burnout Inventory (MBI). Data was collated and held confidentially. Statistical analysis was performed using SPSS.
There were significant associations between certain personality factors of our three cohorts and an increased likelihood of experiencing burnout in run-through training.
The finding that trainees with post-foundation experience of the specialty were less burnt out than those who had gone straight from foundation into a run-through programme needs to be explored further in order to identify possible support strategies.
Further longitudinal work with current respondents may provide more of an insight into Burnout protective mechanisms and coping strategies with respect to personality factors.
With thanks to Daniel Smith, Research and Analytics Manager London Deanery, Information Project Manager COPMeD
1. Ahola, K., Honkonen, T., Kivimaki, M., Virtanen, M., Isometsa, E., Aromaa, A. & Lonnqvist, J. (2006) Contribution of burnout to the association between job strain and depression: the Health 2000 Study. Journal of Occupational and Environmental Medicine 48, 1023–1030.
2. Doherty EM, Nugent E. personality factors and medical training: a review of the literature. Med Educ. 2011; 45(2):132140
3. West et al., (2011) Quality of life, Burnout, Emotional Debt and Medical Knowledge Among Internal Medicien Residents. JAMA. 2011; 306(9): 952-960
4. Modermising Medical Careers. The next steps, The future shape of Foundation, Specialist and General Practice Training programme. April 2004. DOH.
5. Tooke et al., Aspiring to Excellence: Final Report of the Independent Inquiry into Modernising Medical Careers. MMC Inquiry. Aldridge Press. 2008
 Send Email
Send Email