


Theme
eP1 ePosters 1
INSTITUTION
Royal Devon and Exeter Hospital

Background
The transition from medical student to junior doctor requires the graduate to take on a wide range of new responsibilities. They come into a hospital environment which is facing its own challenges; under pressure from increasing admission rates and an ageing and co-morbid patient demographic(1).
These issues may be intensified during out of hours work; an environment in which the junior doctor will find themselves operating within a greatly reduced and often relatively junior team, whilst tackling a large, complex and time-pressured workload.
This transition may be a challenging period both at a personal level for the graduate involved(2,3), and also at a systemic level, where it must be considered as a potential patient safety issue, as the out of hours period has been associated with greater mortality(4). A similar correlation has been noted for the first month of work for new doctors; with a small but significant rise in mortality rates coincident with new doctor cohorts(5,6).
This background was the starting point for the development of the proposed educational intervention designed to improve preparedness of medical students for out of hours work.
Prior to the construction of the resource, it was felt a deeper understanding the process of transition faced by new graduates was required. To this end, a systematic collation of the qualitative research surrounding the preparedness of medical graduates for out of hours work was carried out, asking the following question: What skill areas do new graduates and other healthcare workers identify as important for out of hours working?
Following this, the resource was developed, taking the form of a series of interactive cases placed within the framework of an online simulated on call environment.
Its development was an iterative process adapted based on feedback from students and junior doctors as to usability and usefullness. The resulting resource and the rationale behind it are discussed in further detail below.
Results of qualitative synthesis
Analysis of 10 papers meeting inclusion criteria revealed several important themes; dealing with uncertainty, responsibility and isolation, communication and team working, time management, practicalities of working in the hospital environment, and prescribing (see details tab for further analysis).
These were synthesised into two dimensions that link these topics and help inform development of educational interventions. First, is the key role that the transition of identity plays in commencing post.The development of this identity requires that learning is experiential with a degree of controlled responsibility placed on the student. Second is the development of the ability to work in a complex and imperfect environment - in the sense of both the wider hospital system, and in tackling clinical scenarios that are less clearly defined both in their framing and outcomes.
The resource
Simulated environment
The level of realism of the simulation was carefully considered given the technological and resource constraints to be worked with. The system in place is based on a 2D text and image system whereby different cases are based on different webpages, navigable in any order by the student. The realism was focused on receiving and attending jobs, given that in the context of an on call, one of the most unfamiliar and psychologically stressful aspects is dealing with multiple patients at once(7, 12). A further contextual element is provided by the use of an on screen clock - choosing certain optional further investigations will advance this clock by an appropriate amount of time. A concern in testing was that this aspect could promote maladaptive strategies whereby students try to work to the clock rather than the clinical situation. Therefore there is no 'reward' for taking less time - it is simply to place the cases in context, and to encourage careful consideration prior to the ordering of tests.
The cases
Based on the outcomes of the qualitative background work for this resource, it was clear that the cases needed to be designed to allow the students to make their own decisions, unguided by a multiple choice framework, in scenarios where a question was not precisely defined. The case content was determined through discussion with junior doctors as to commonly encountered scenarios. The response framework is the same for each case, and designed to mimic reality - the students is asked to record an assessment and plan in the notes, to prescribe as appropriate, and to choose how they would escalate the issue if required. This clearly requires a greater time investment on behalf of the student, but in testing was felt to be of greater learning benefit than answering a set of pre-defined closed questions.
Feedback
Students currently receive feedback after the on call has ended - with exemplar notes and prescriptions as well as further information and links to outside resources displayed side by side with their own actions. Following testing, the exemplar choice of case escalation was removed - as it was felt this would depend on the individual context. Students are also provided with information as to how long they took to attend scenarios, stratified by how urgent they felt them to be.
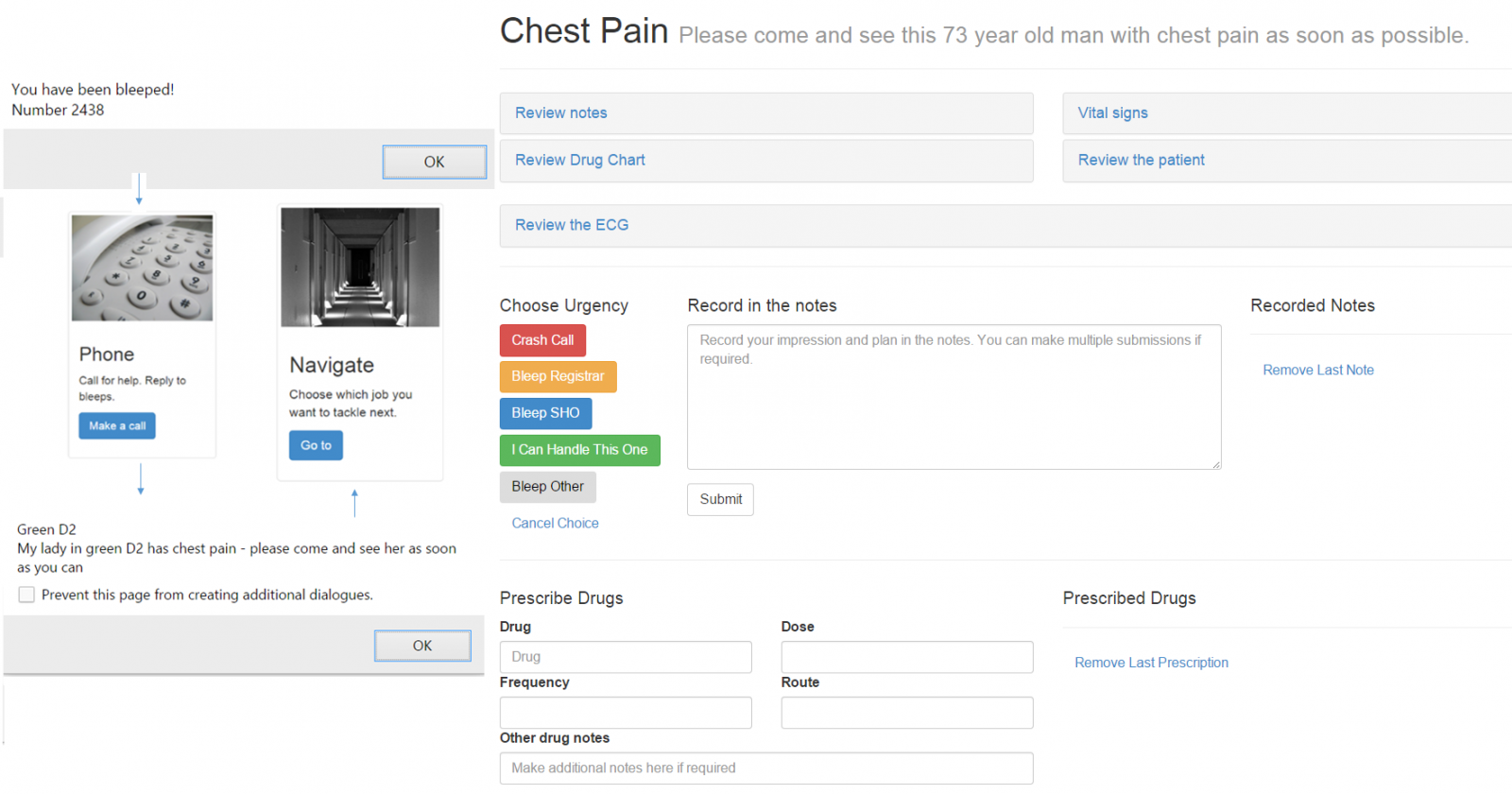
An online simulated on call environment has been designed and pre-piloted.
Further evaluation is to take place in the coming academic year. The simulator has te capability to store responses made by students, so that the quality of their prescriptions and notemaking may be tracked over time. This is to be complemented by questionnaire data into perceived usefulness and enjoyment. Interviews will be carried out based on the background qualitative review carried out prior to resource development to guage whether the simulator has had an impact on student learning and preparedness for out of hours practice.
- On call work is a challenging area for new graduates and should be a focus of learning for senior medical students.
- Simulation may be a safe and effective tool for allowing students to develop their clinical decision making and responsibility in a more complex and uncertain environment.
- A novel simulated on call environment may be accessed at: http://simulator.ngrok.com/On%20Call%20Simulator/src/homepages/index.html
- Hospitals on the edge? The time for action [Internet]. Royal College of Physicians; 2012 Sep p. 8. Available from: https://www.rcplondon.ac.uk/sites/default/files/documents/hospitals-on-the-edge-report.pdf
- Bogg J, Gibbs T, Bundred P. Training, job demands and mental health of pre-registration house officers. Med Educ. 2001 Jun;35(6):590–5.
- West CP, Shanafelt TD, Kolars JC. Quality of Life, Burnout, Educational Debt, and Medical Knowledge Among Internal Medicine Residents. Jama-J Am Med Assoc. 2011 Sep 7;306(9):952–60.
- Aylin P, Yunus A, Bottle A, Majeed A, Bell D. Weekend mortality for emergency admissions. A large, multicentre study. Qual Saf Health Care. 2010 Jun;19(3):213–7.
- Jen MH, Bottle A, Majeed A, Bell D, Aylin P. Early In-Hospital Mortality following Trainee Doctors’ First Day at Work. PLoS ONE. 2009 Sep 23;4(9):e7103.
- Phillips DP, Barker GEC. A July Spike in Fatal Medication Errors: A Possible Effect of New Medical Residents. J Gen Intern Med. 2010 May 29;25(8):774–9.
See 'more detail' tab for references from the qualitative review.
 Send Email
Send Email